Arthritis is one of the most common causes of pain in the hip. Arthritis is a progressive disorder, which means that it typically starts gradually and gets worse with time. The term arthritis literally means “inflammation of the joint.”
There are different types of arthritis that can affect the hip. The type of arthritis you have may affect your treatment options.
Types of Arthritis
There are five main types of arthritis that can affect the hip joint. They are:
- Osteoarthritis
- Rheumatoid arthritis
- Ankylosing spondylitis
- Systemic lupus erythematosus
- Psoriatic arthritis
There is no cure for any type of arthritis, but there are ways to treat the pain and other associated symptoms.
Osteoarthritis
Osteoarthritis means “arthritis of the bone” and is the most common form of arthritis. It is often described as the result of wear and tear on the joints, which explains why it is more common in older than younger people.
The hip joint consists of the ball-shaped end of the thigh bone (femoral head) which fits into the hip socket (acetabular socket). The inside of this ball-and-socket joint is lined with smooth cartilage to help the joint move easily. If this smooth cartilage wears away, the remaining rough surfaces of the ball-and-socket grind against each other, causing pain. Over time, osteoarthritis can degenerate or permanently damage the joint.
Osteoarthritis of the hip (and other parts of the body) has been associated with the following:
- Structural problems with the hip joint (hip dysplasia, femoroacetabular impingement)
- Advancing age
- Obesity
- Previous damage or injury to the hip
However, osteoarthritis may develop in people without these risk factors.
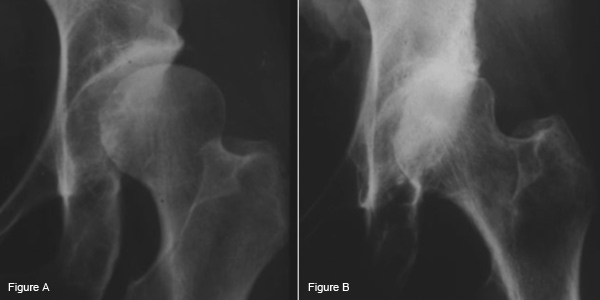
Two radiographs of a female patient showing acetabular dysplasia (a shallow hip socket). The patient started to have hip pain when she was 20 years old (a). This hip dysplasia was not treated and 15 years later she had end-stage osteoarthritis of the hip (b). Note the complete loss of cartilage joint space between the ball and the socket over this 15-year interval.
Rheumatoid Arthritis
Rheumatoid arthritis is a systemic disorder, that is, it affects your entire body and not just the hip joint. The inflammation is related to an immune system response rather than wear and tear.
The hip joint, like other joints in the body, is protected by a special capsule that completely surrounds the joint. This capsule has a special lining (the synovial lining) and is filled with lubricant (joint fluid) that helps the joint move smoothly. Rheumatoid arthritis typically causes a swelling of the synovial lining. This causes pain and swelling, but eventually, rheumatoid arthritis can cause the bone and cartilage of the joint itself to deteriorate.
Rheumatoid arthritis can occur in people of all ages, including children (where it is known as juvenile rheumatoid arthritis), and is more common in women than men. Unlike osteoarthritis of the hip, which may occur only in one hip, rheumatoid arthritis typically occurs in both hips at the same time (and possibly other joints). Rheumatoid arthritis is also associated with overall weakness and fatigue. Medications to treat rheumatoid arthritis continue to improve.
Ankylosing spondylitis
Ankylosing spondylitis is a chronic inflammation of the spine and sacroiliac joint (the joint where the spine meets the pelvis) which can sometimes cause inflammation of the hip joint. Ankylosing spondylitis can occur in people of all ages, including children, and typically starts in a person between the ages of 17 and 35. It is more common in men than women.
It is typical for people with ankylosing spondylitis to experience flares, when the condition is worse, followed by periods of remission with mild to no symptoms.
Systemic Lupus Erythematosus
Systemic lupus erythematosus or lupus is a systemic autoimmune disorder that can affect any part of the body, including the hip joint. If lupus strikes the hip, inflammation and damage to the joint can occur. Lupus can occur in people of all ages but it is most common in women aged 15 to 35.
Psoriatic Arthritis
As the name sounds, this type of arthritis is related to the skin condition psoriasis. Psoriatic arthritis causes joint pain, swelling, and stiffness and can affect any joint in the body, including the hip. Most people with psoriatic arthritis have the skin condition first (scaly red patches of skin) but it is possible to develop psoriatic arthritis before the skin condition occurs.
Arthritis Symptoms
Regardless of the type of arthritis, symptoms of hip arthritis include:
- Pain in the hip joint that may include pain in the groin, outer thigh, or buttocks
- Pain that is typically worse in the morning and lessens with activity
- Difficulty walking or walking with a limp
- Pain that worsens with vigorous or extended activity
- Stiffness in the hip or limited range of motion
In patients with rheumatoid arthritis or lupus, fatigue and weakness may also occur. Arthritis often occurs in flares with remission, but some people experience a relatively stable level of pain without flares.
Any type of arthritis can involve more than one joint in the body, so a person with osteoarthritis of the hands may develop the condition in the hip as well. Rheumatoid arthritis and lupus typically affect both hips at the same time, while osteoarthritis and psoriatic arthritis may occur in one hip but not the other.
Diagnosis
If you suspect you may have arthritis of the hip, the most important first step is an accurate diagnosis. Dr. Clohisy and his colleagues are experts in arthritis of the hip. A diagnostic evaluation will likely include the following:
- Your medical history, including where you experience pain and if you limp at times
- A physical examination, in particular to see how well you can move the hip
- Radiographs or X-rays to determine if there are any abnormalities in the joint
- Blood tests to determine antibodies that may be associated with a specific type of arthritis (only if needed).
Treatment
Dr. Clohisy and his colleagues will prescribe the type of treatment that is appropriate for your particular type of arthritis and other factors, including your overall health, your age, and your personal preferences.
Nonsurgical treatment of arthritis of the hip may include any of the following:
- Anti-inflammatory medications, such as ibuprofen
- Corticosteroids, injections to block the inflammation in the joint
- Physical therapy or exercise programs to improve flexibility, build up strength, and maintain muscle tone. Swimming, in particular, is an excellent exercise for arthritis sufferers.
- Some types of arthritis may respond to new categories of drugs known as symptom-modifying antirheumatic drugs (SMARDs) and disease-modifying antirheumatic drugs (DMARDs). These are powerful new drugs, which are not appropriate for everyone with arthritis.
- Devices such as canes or walkers to make it easier and safer for you to walk.
Lifestyle modifications can also help to reduce the symptoms of arthritis of the hip. These include:
- Maintaining a healthy weight (and losing weight, if necessary)
- Appropriate pain management
- Changing activities to minimize stress on the hip
- Exercising to build up strength
Many people with arthritis with the hip are candidates for surgery. Surgery can help to reduce pain, enhance quality of life, and improve your ability to perform everyday activities with fewer or no restrictions.
- Total hip replacement may be appropriate if the hip joint is severely damaged
- Osteotomy surgery may be appropriate in less severe cases. Hip osteotomy procedures reposition the joint surfaces in such a way that it allows the healthy part of the hip joint to bear most of the body’s weight. Only a select group of patients are candidates for osteotomy surgery.
If you are an appropriate candidate for hip surgery, the risks and benefits of your surgical options will be discussed.
Important Considerations for People with Arthritis of the Hip
There is no cure for arthritis. Typically, it starts gradually and worsens over time. Eventually, all forms of arthritis of the hip may permanently damage the hip joint. While osteoarthritis is more common in older people, there are forms of arthritis that affect younger people.
Fortunately, there are things that can be done to help minimize the effect of arthritis, and we are glad to discuss these options.
Arthritis Statistics
- 22% of the U.S. population in 2010 reported some form of arthritis
- Among adults over 65, 50% have some form of arthritis
- The most common form of arthritis is osteoarthritis
- Weight loss of just 11 pounds can reduce a woman’s risk of developing knee arthritis by 50%
- Of working age people (ages 18 to 64), one-third of those who had arthritis reported it limited their ability to work
(Statistics from Centers for Disease Control and Prevention)